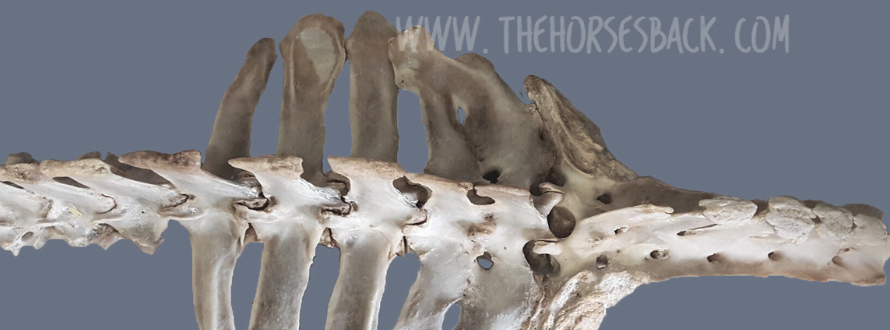
This post on the early treatment of ‘crooked legs’ in foals (Angular Limb Deformities) is written by Dr Lauren Jones, the veterinarian behind Kentaro Veterinary Services, a mobile equine practice on the Coffs Coast of NSW, Australia.
Known for her calm, practical approach, Lauren spends her days helping horses from foals to elite eventers. She’s passionate about education, preventative care, and the demystification of veterinary medicine, giving owners clear, no-nonsense advice they can actually use.

Dr Lauren writes:
Ever had someone say your horse is duck-footed or pigeon-toed? Or maybe that they paddle or have a wonky gait?
That’s often due to a conformational fault. The good news is that in foals, it’s something we can often correct before it becomes a long-term problem.
There are all types of these – legs that bend in, out, or are contracted or lax. Each type changes the way the joints line up and the way forces travel down the limb.

This is exactly why I’m so particular about foal checks at birth. Early intervention gives us the best chance to guide those growing legs into alignment.
It’s never a one-person job – it takes a team effort: dedicated owners, a skilled farrier, a bodyworker, and a vet with an eye for detail. Together we can make a huge difference in how that foal matures and moves for life.
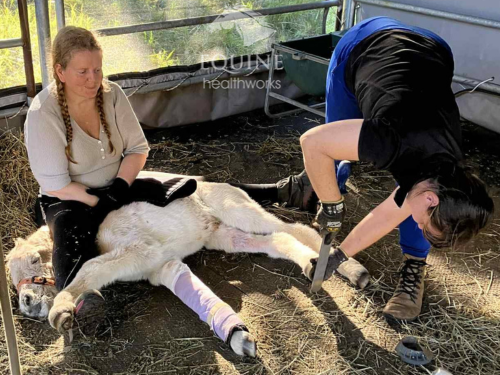
A quick run-down on those crooked legs
Angular Limb Deformities (ALD) can look like a foal doing the hokey kokey, but what’s really happening is much more complicated. These deformities come in a few different flavours and can be congenital (born that way) or acquired (develop after birth).

Congenital causes
These are usually linked to what happens before or around birth.
- Soft tissue trauma during delivery.
- Lax or flaccid joints, when the ligaments and tendons are just a bit too stretchy at birth.
- Premature birth, twin pregnancies, placentitis, etc. can cause underdeveloped bones (incomplete ossification)

Developmental (acquired) causes
These are termed ‘acquired’. They tend to show up a bit later and are often influenced by:
- Unbalanced nutrition (too much, too little, or the wrong mix for growing foals).
- Excessive exercise or trauma – those young legs take a lot of load too quickly.
- Environmental factors – a hill can cause a slant if a foal is already tending one way or another.
- Lack of good hoof care early can lead to abnormal wear, changing the forces on the foot.
Some of these can be sneaky and hard to spot until the foal hits the ground and starts moving.

In simple terms, we talk about:
- ‘Valgus’ is when the limb angles outwards (toes point out, knees or hocks in).
- ‘Varus’ is when the limb angles inwards (toes point in, knees or hocks out).
- Contraction is when everything is too tight.
- Laxity is when everything is too loose.
- A combination of all the above.

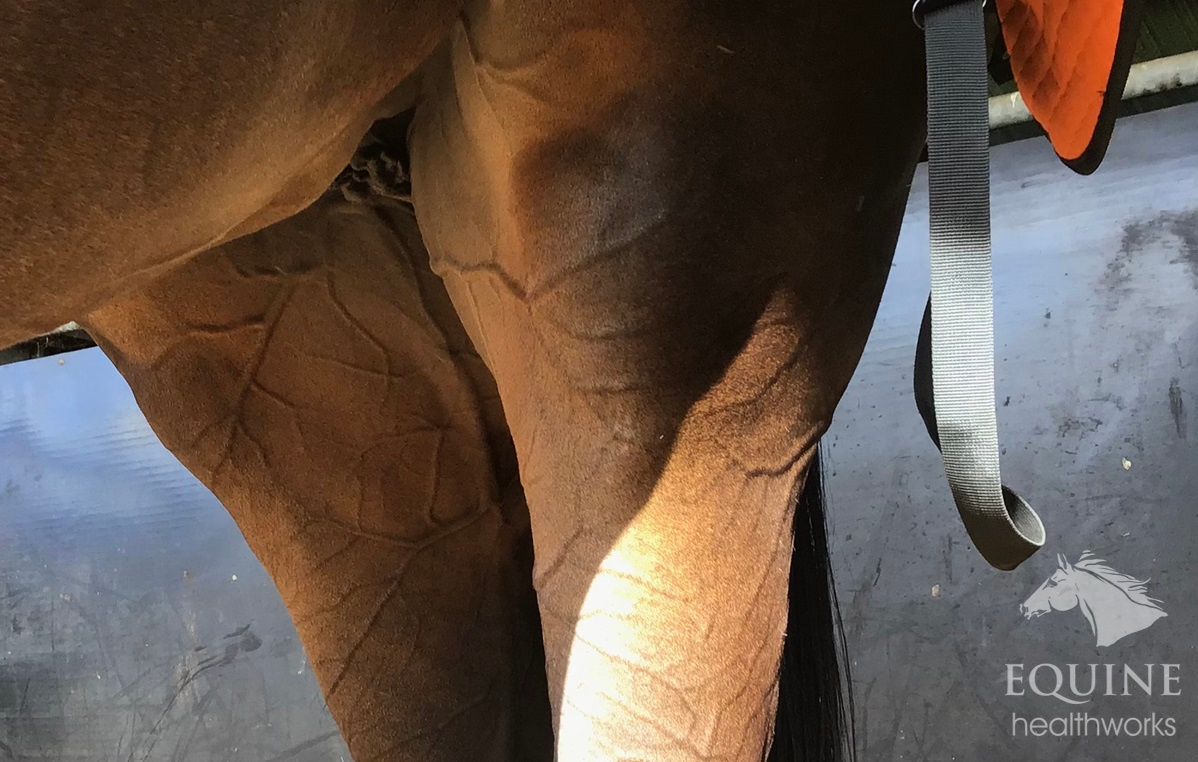
And ever seen a little foal that looks like the wind’s been blowing from one side a bit too long? Meet the windswept foal – a classic example of Angular Limb Deformities in action. This foal is half Valgus, half Varus. You put your left foot in and your right foot out and shake it all about…
Straight talk about treatment
Every foal is different, and the key is working out whether that crooked leg needs a bit of time, a trim, or a team approach to get things straight again.
The good news? With the right plan and good teamwork, these cases can do brilliantly, and what’s more, they do so in a pretty short period of time.
Here’s how we can tackle mild to moderate limb deformities with conservative management. For more severe cases, surgical management is an option.
Exercise-restriction or controlled exercise
When the muscles are too tight, then we need to rest them to let them relax. When the muscles are too loose, they need gentle exercise to strengthen them.
Corrective trimming
Our farrier team works magic here! Small, frequent trims can help rebalance how the foot hits the ground and redirect forces up the limb.
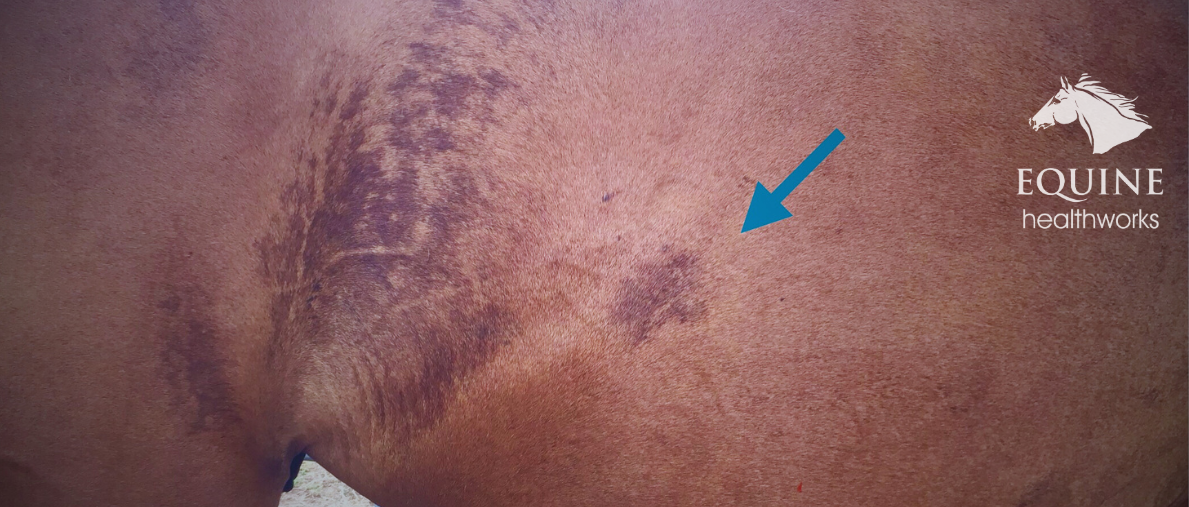
Here we are looking at left-to-right imbalances. When you pick up the foot of a pigeon-toed horse, you will notice that one heel is longer than the other. The first step is to even the heels up (it can be millimeters), before reassessing.
If the fetlock is straight, great! If not, we can come back and take off a couple more millimeters. Be wary, as there isn’t much foot to play with. It’s best to do this trimming under an experienced eye.

Hoof extensions
Glue-on or lightweight extensions can shift the weight distribution and give growing bones a little nudge in the right direction.


Physio tape
This fires the nerves to work more on one side than the other, due to gentle tactile feedback. This can encourage the muscles to work slightly harder on one side in order to straighten the leg.

Splints and bandages
Used carefully and for short periods, these help support weak or lax joints while the soft tissues strengthen. They can also be used to gently stretch tight joints. Note: these look simple, but are not without risk, as they can heat up the leg, slip, or cause rub. It’s very easy to end up with long-lasting scar tissue and white hair. If used incorrectly or if the foal is too boisterous, they can cause negative effects quickly!
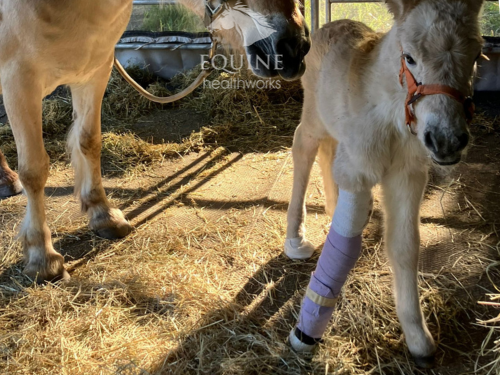
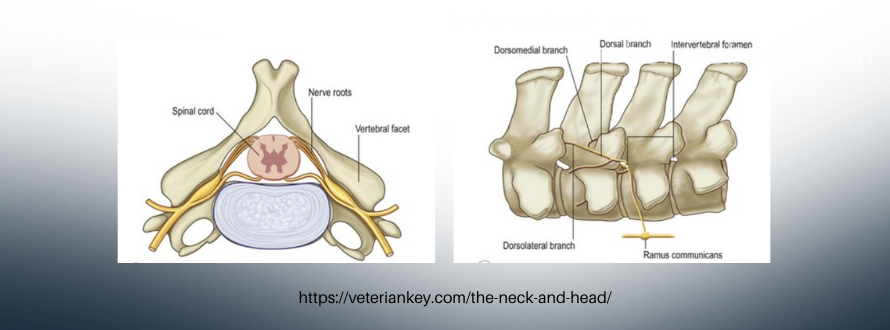
Bodywork
Some gentle bodywork, including a little limb mobilisation and stretching, or acupuncture can help ease the muscular tensions that build up as the foal works hard to balance itself. Some modalities will stimulate the nervous system and help it to ‘forget’ the incorrect posture as the limbs improve.
Surgery
For more severe or stubborn cases, we can use veterinary surgery. ‘Stripping’ is when the bone membrane is lifted to speed growth on the ‘short’ side of the leg. ‘Stapling’ is when a screw or pin is fixed across the growth plate to slow growth on ‘long’ side of leg. That’s how surgery influences bone growth. It’s a higher level of intervention, but timing is still critical.
Should your foal be confined or not?
Owners are often ‘advised’ by well-wishers that they should keep their foal confined, or allow it to run around to exercise – with the same advice being given for all manner of Angular Limb Deformities.
Try not to take such advice, but instead get a vet with an experienced eye for forelegs AND hindlegs to have a look at mare and foal in the first 12 to 24 hours. Doing so gives many advantages.
For the mare, we check that:
- She has passed her membranes,
- Her udder is comfortable,
- Any minor tears are treated.
We can also assess whether she is going to need a post-foaling flush treatment.

For the foal, we check that:
- Meconium has passed normally,
- The bite is strong,
- The heart has no murmurs,
- The lungs are clear,
- The umbilicus is clean and dry,
- There are no hernias,
- Temperature is normal.
We also do an IGG test to check the immune system has absorbed enough antibodies from mum’s first milk, which carries colostrum.
Importantly, we check legs for straightness and development, seeing problems that the owner might not spot. We create a plan if they need treatment.
It’s best to keep both mum and foal confined until then! This also has another advantage: the pair bond in a safe place so that mum doesn’t need to get over-protective or run from that ‘lion’, over-exercising those vulnerable baby legs.
Be sure to act in time
No matter the approach, monitoring is critical. Foals grow fast, sometimes changing week to week, and what’s perfect timing for one joint might be too late for another.
Don’t leave it too late! Fetlock deformities are best addressed before 4 months of age, as growth plates near closure. The window for knee and hock deformities is longer, but the best results are achieved before 6-8 months.
Where possible, early management is nearly always better, as you’ll see faster results for less intervention. It also leaves less time for problems to worsen or lead to additional issues.
That’s why early checks and ongoing follow-up visits make all the difference to your growing foal’s legs.